Benign Oncocytic Neoplasm of the Right Parotid Gland in a 45-Year-Old Male
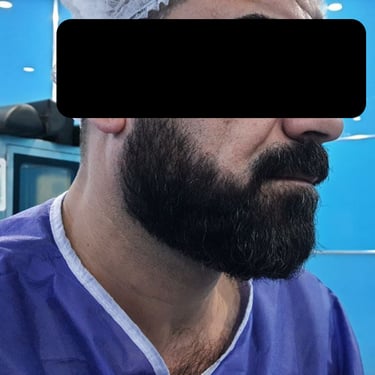
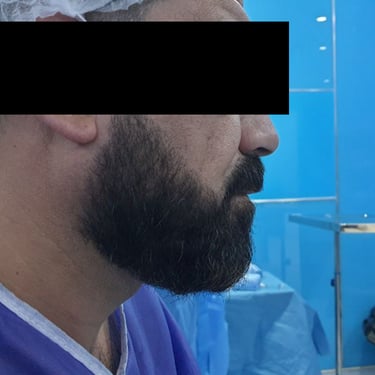
A 45-year-old male presented with a two-year history of right infra-auricular swelling. The mass was associated with decreased hearing on the right side, intermittent pain radiating to the tongue, and reduced salivary output. There were no systemic complaints such as weight loss or night sweats. His past medical history was unremarkable, except for a remote appendectomy performed without complications. The patient had no history of chronic medication use, although he reported a previous allergic reaction to an unidentified intravenous medication given during a flu-like illness.
SURGERYHEAD AND NECKVIDEO
8/11/20252 min read

A 45-year-old male presented with a two-year history of right infra-auricular swelling. The mass was associated with decreased hearing on the right side, intermittent pain radiating to the tongue, and reduced salivary output. There were no systemic complaints such as weight loss or night sweats. His past medical history was unremarkable, except for a remote appendectomy performed without complications. The patient had no history of chronic medication use, although he reported a previous allergic reaction to an unidentified intravenous medication given during a flu-like illness.
Initial Imaging and Fine Needle Aspiration Cytology:
Ultrasound of the neck and right parotid gland demonstrated a mildly enlarged right parotid with a well-defined, solid, hypoechoic nodule measuring 32 × 20 × 16 mm, located at the mid to lower third of the gland and involving both the superficial and deep lobes. The lesion showed mild peripheral vascularity and was interpreted as a likely salivary gland tumor. Both lobes of the thyroid appeared normal with homogeneous echotexture and no focal lesions. Bilateral level I cervical lymph nodes were observed, the largest being a 39 × 8 mm node in the right submandibular region; all nodes demonstrated preserved hilum and were hypovascular with cortex <4 mm—features not concerning for malignancy. The submandibular glands were unremarkable bilaterally.
Fine needle aspiration (FNA) of the parotid lesion was performed, and cytological analysis revealed oncocytic features. According to the Milan System for Reporting Salivary Gland Cytopathology, the diagnosis fell under Category IVa — “Neoplasm: favoring benign.” The cytologic impression was consistent with an oncocytic neoplasm, most likely a Warthin tumor.
Preoperative Workup and Surgical Management:
Routine preoperative blood tests were within acceptable limits, including a serum urea of 36.4 mg/dL, creatinine of 1.35 mg/dL, and serum glucose of 91.2 mg/dL. Viral screening tests were negative. The patient was scheduled for definitive surgical excision of the mass.
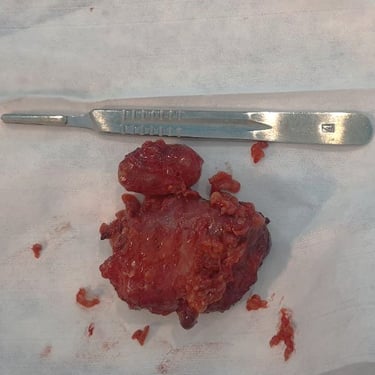
A right total conservative parotidectomy was performed under general anesthesia. The patient was positioned supine with the neck extended. A modified lazy-S incision was made to access the gland. The parotid gland was carefully dissected and excised with preservation of the facial nerve and its branches. Hemostasis was achieved, and a corrugated drain was placed. The wound was closed in layers without intraoperative complications.
Histopathology Report – Initial Surgery:
Histopathological evaluation confirmed the diagnosis of a Warthin tumor. The mass was well-circumscribed with pushing borders and composed of papillary epithelial projections lined by a characteristic double layer of oncocytic epithelial cells. The cytoplasm was abundant and eosinophilic, and the supporting stroma contained dense lymphoid tissue with germinal center formation. Surrounding salivary tissue was unremarkable, and no evidence of malignancy was found. Reactive lymph nodes were also noted within the specimen.