Dermatofibrosarcoma protuberans 5 times recurrence: A case report of a 61 years old male
An 61-year-old male from Sulaymaniyah, Iraq, presented with palpable hardness for about 2 months on the left chest wall at the site of previous operation with no significant past medical history. He has undergone 4 previous operations at the same site for the same condition, and also received radiotherapy, not a smoker. With no significant family history of the same condition or other malignancies.
SURGERY
6/17/20253 min read
Patient Information:
An 61-year-old male from Sulaymaniyah, Iraq, presented with palpable hardness for about 2 months on the left chest wall at the site of previous operation with no significant past medical history. He has undergone 4 previous operations at the same site for the same condition, and also received radiotherapy, not a smoker. With no significant family history of the same condition or other malignancies.
Clinical Findings:
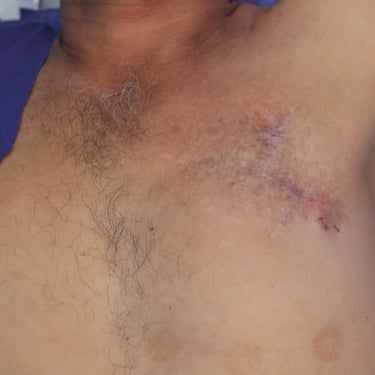
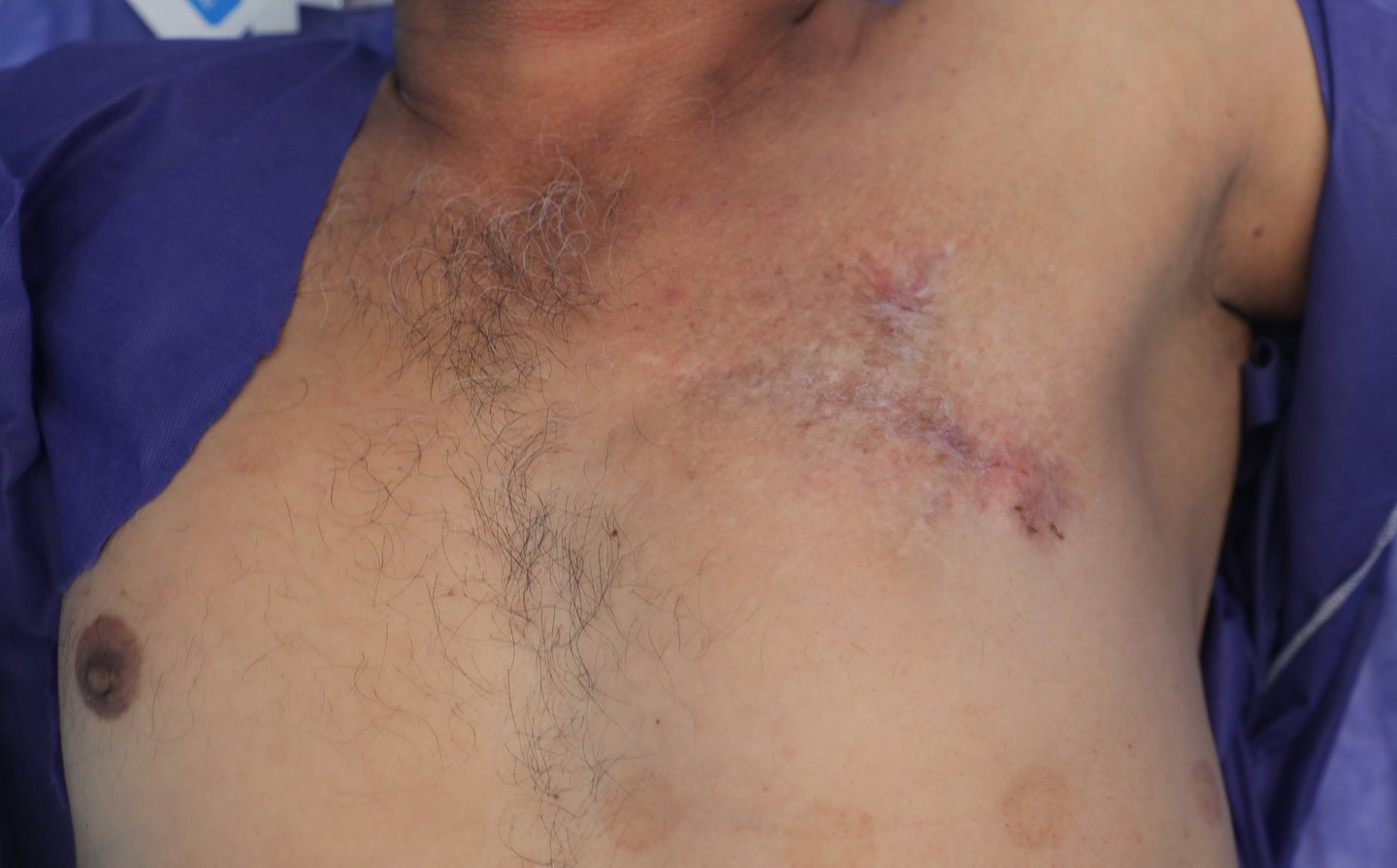
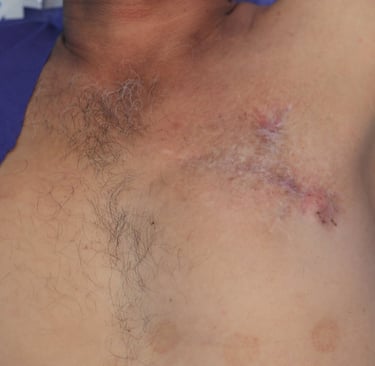
On inspection of the left anterior chest wall, within the region of the male breast, a linear postoperative scar measuring approximately 10 cm was observed. A second, shorter transverse scar measuring 3–5 cm with a fibrinous base was noted above the primary incision. The overlying skin appeared dry, with erythematous to violaceous plaques, telangiectatic vessels, and a hardened, elevated surface, particularly around areas of prior surgical manipulation. On palpation, two subcutaneous masses were palpable along the horizontal scar. One was located at the lateral edge and the other at the midpoint. Both lesions were firm, irregular, non-tender, and fixed to underlying structures, with poorly defined margins. The lateral mass was slightly larger than the central one. The nipple-areolar complex was absent, consistent with the previous surgical resection. Palpation confirmed adherence of the mass to the underlying pectoral musculature.
Diagnostic Approach:
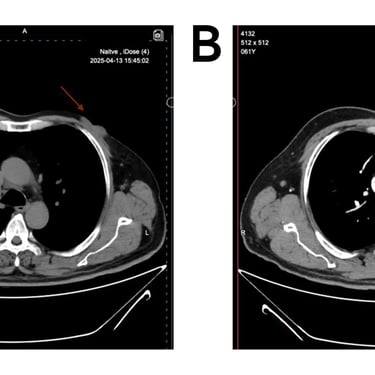
In 2003 a small lesion progressively evolved into a vascularized, tender mass exhibiting epidermal atrophy and contact bleeding. Core biopsy showed Dermatofibrosarcoma protuberans. Contrast-enhanced computed tomography (CT) showed localized disease without evidence of metastasis. The patient underwent surgical excision histopathology diagnosis also confirming Dermatofibrosarcoma protuberans, followed by adjuvant radiotherapy consisting of 20 sessions. The patient had previously undergone four local excisions for recurrent DFSP. Notably, these recurrences occurred annually during Ramadan between 2022 and 2024, every time the Histopathological examination confirmed the diagnosis of Dermatofibrosarcoma protuberans, with a fifth time emerging in the pre-Ramadan period of 2025. The most recent lesion prompted delayed post-holiday evaluation. High-resolution ultrasound of the chest wall revealed two focal cystic lesions with internal hyperechoic echoes—one measuring 24 × 10 mm in the lateral aspect corresponding to a skin bulge, and another 15 × 5 mm just medial and inferior to the first, both suspicious for local recurrence. Contrast-enhanced CT scan of the chest and abdomen was performed ( a 4.3 cm left chest wall mass with a 1.2 cm thickness, broad contact with the pectoralis major muscle, and possible muscle invasion, No pathological lymphadenopathy was identified in the axillary or internal mammary chains, and no distant metastasis was detected ) Figure 2(A) & ( B).
Therapeutic Intervention:
Due to the aggressive nature and deeper invasion of the fifth recurrence, a more extensive surgical approach was employed. Wide local excision was performed, including en bloc resection of the underlying pectoralis major and minor muscles as well as the fifth rib Figure1 ( B ) & ( C ) & ( D ). Intraoperatively, pleural involvement necessitated the placement of a chest tube for postoperative drainage . The resulting defect was reconstructed using a local rotational flap Figure 1 ( E ). Histopathological examination of the excised specimen showed recurrent DFSP., The tumor exhibited no lymphovascular invasion, and resection margins were negative with no evidence of high-grade transformation. Immunohistochemical staining demonstrated ( diffuse, strong membranous positivity for CD34, while Desmin, SMA, and SOX10 were negative). The patient was subsequently referred to a multidisciplinary oncology team for further management, including evaluation for systemic therapy and long-term surveillance.
Follow-Up and Outcome:
Postoperatively, the patient attended regular follow-up visits to monitor wound healing, flap viability, and shoulder function. The chest tube was removed on postoperative day 2, the closed passive drain was put and removed after 3 days. The patient was advised to limit ipsilateral shoulder movement for two weeks to facilitate wound healing. Sutures were removed during follow-up, and the recovery period was uneventful.
Figure Legend:
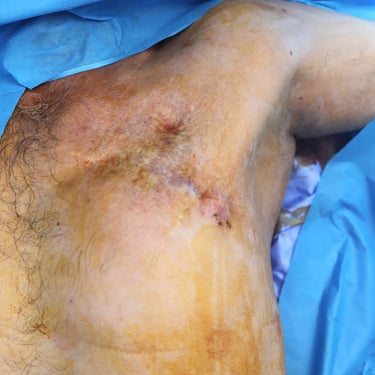
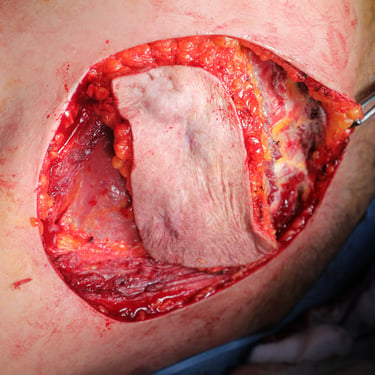
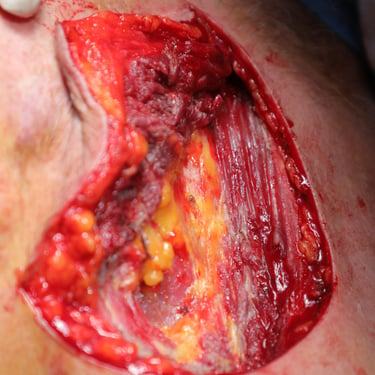
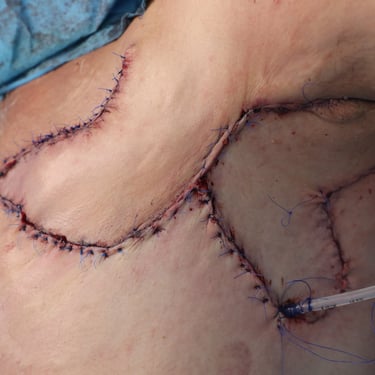
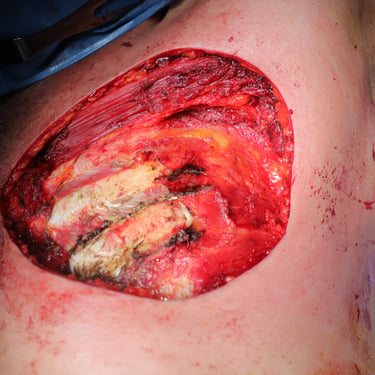
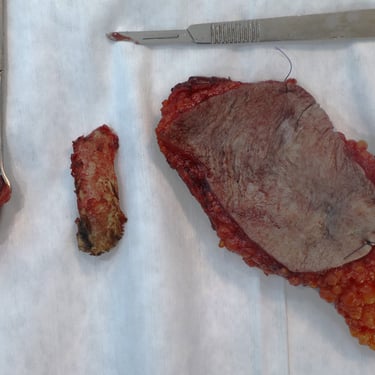
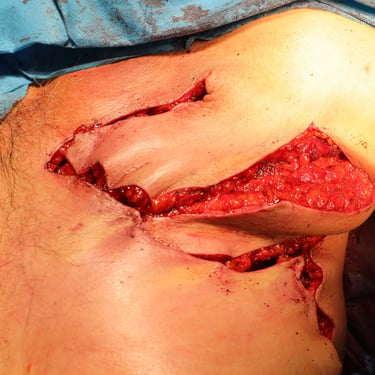
Figure 1. (A) Preoperative clinical image showing the left anterior chest wall with post-surgical scarring, dermal atrophy, and subtle violaceous discoloration overlying the recurrent lesion site.(B) Intraoperative view following wide local excision, revealing exposure of the underlying pectoral muscles with tumor invasion extending to the chest wall.(C) Resected specimen including the mass and overlying skin and subcutaneous tissue (left), excised fifth rib (center), adherent deep tissue and pectoralis muscle (right).(D) Immediate postoperative result following wide local excision and reconstruction with local advancement flap. A drain is visible at the inferior margin of the incision.(E) Postoperative follow-up showing flap viability, intact sutures, and early stages of wound healing with no evidence of complications.
Figure 2. (A) CT scan -Axial native and (B) contrast enhanced show an enhancing soft tissue density in the left breast (red arrows) invading pectoral muscles, with out rib destruction, no axillary lymph nods enlargement.
Limitations:
Genetic testing for the COL1A1–PDGFB fusion gene was not performed in this case, its assessment could have provided additional molecular confirmation and therapeutic insight, particularly regarding eligibility for targeted therapy with imatinib in the context of recurrent disease. But the patient couldn't do it due to the high cost.
Gallery