Management of a 50-Year-Old Female with Palpitation, Weight Loss, Eye Protrusion, and Incidental Parathyroid Adenoma
A 50-year-old female presented with palpitation, weight loss, and eye protrusion. Her past medical history is unremarkable, apart from hyperthyroidism for the past eight years while taking anti-thyroid medications. She has no surgical history.
SURGERY
7/14/20242 min read
Case Presentation:
A 50-year-old female presented with complaints of palpitation, weight loss, and eye protrusion. Her past medical history was notable only for hyperthyroidism, which she had been managing with anti-thyroid medications for the past eight years. She had no history of prior surgeries or other significant health issues.
Laboratory Details:
The following laboratory results were obtained:
Thyroid-Stimulating Hormone (TSH): 0.25 µIU/mL
Free T4 (FT4): 19.0 pmol/L
TRAb (TSH Receptor Antibodies): 13 IU/L
Blood Urea: 25.5 mg/dL
Serum Creatinine: 0.79 mg/dL
These results, particularly the low TSH and elevated FT4, supported the diagnosis of hyperthyroidism, likely associated with Graves' disease, given the presence of eye protrusion.
Imaging Studies:
Neck Ultrasound Findings:
Thyroid Gland: Normal in size but showed heterogeneous echotexture with a few small nodules (<7 mm in both lobes, TI-RADS 3). There was a mild increase in the vascularity of the gland with no micro or macro-calcifications, suggesting Graves' disease.
Parathyroid Gland: No clear mention of abnormal findings in the parathyroid during ultrasound, suggesting the presence of a hidden incidental finding.
Treatment Strategy:
Given the diagnosis of hyperthyroidism and the ultrasound findings consistent with Graves' disease, the patient was scheduled for total thyroidectomy to manage the hyperthyroidism and potential thyroid pathology.
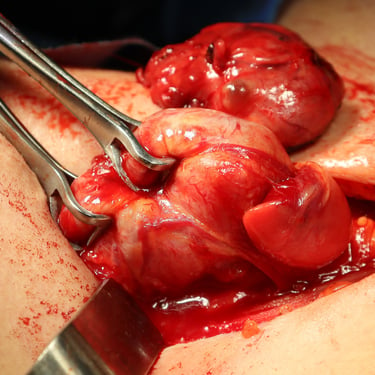
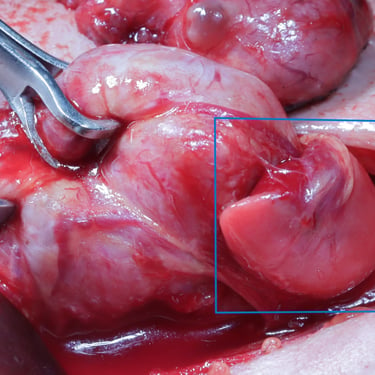
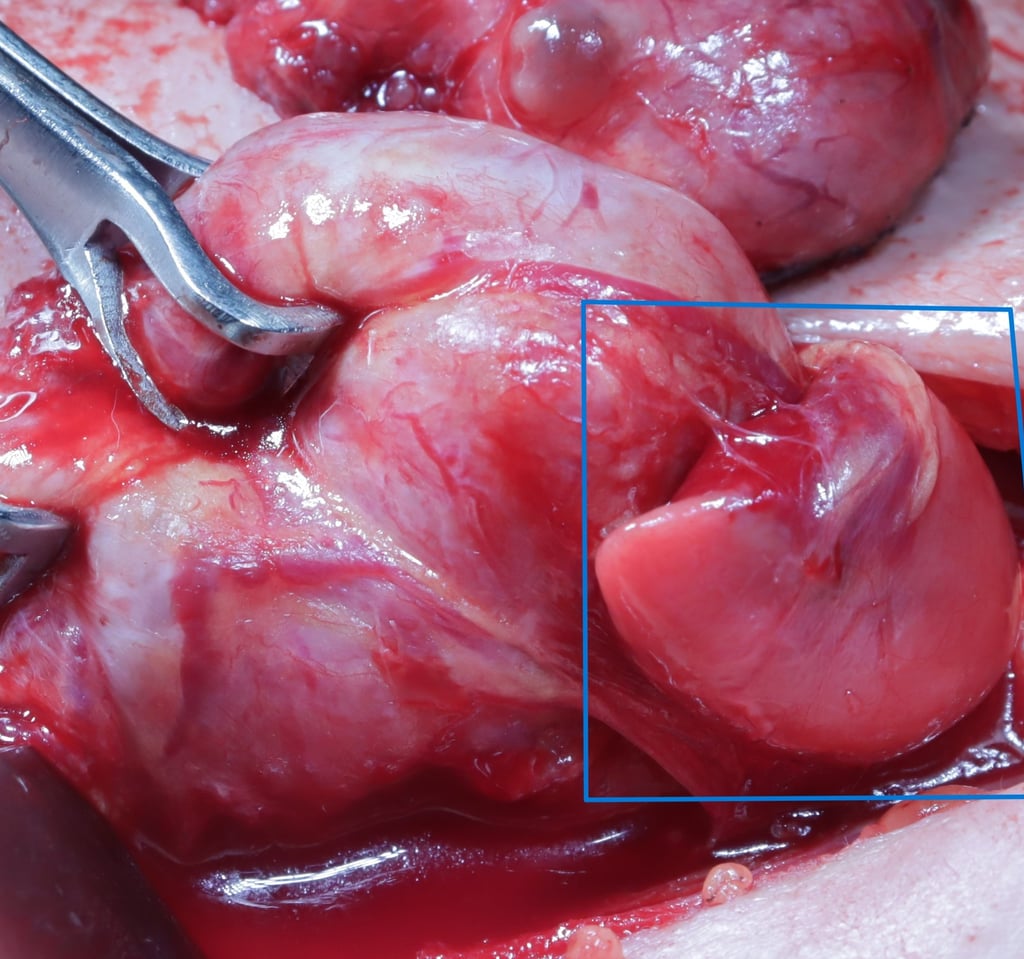
Surgical Intervention:
During the surgery, a sizable mass was noted in the lower portion of the right thyroid lobe. This mass was carefully excised along with the thyroid gland, and sent for histopathological examination.
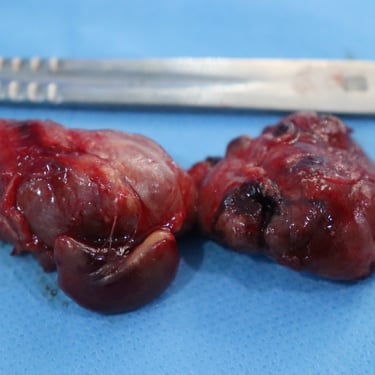
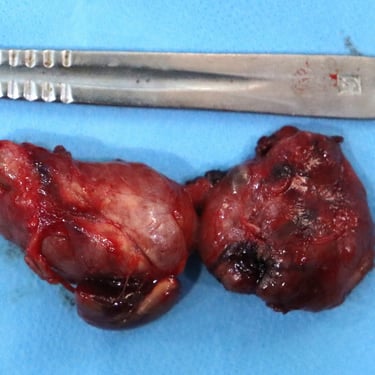
Histopathological Examination (HPE):
The histopathology report revealed two key findings:
Graves' disease, as expected based on the clinical presentation.
An incidental parathyroid adenoma was found in addition to the thyroid pathology. This was an unexpected but clinically significant finding.
Discussion:
This case highlights the importance of thorough surgical exploration and histopathological examination in patients undergoing thyroid surgery. While the patient initially presented with classic symptoms of hyperthyroidism and Graves' disease, the incidental discovery of a parathyroid adenoma during thyroidectomy emphasizes the need to be vigilant for coexisting pathologies, especially in cases of long-standing thyroid disorders.
Parathyroid adenomas are typically benign and often asymptomatic. However, when they become symptomatic, they can lead to hyperparathyroidism, which may cause a variety of symptoms such as fatigue, depression, and bone pain. In this case, the adenoma was discovered incidentally, and no signs of hyperparathyroidism were present in the patient’s lab results. Nevertheless, the presence of the adenoma warrants follow-up to monitor for any future symptoms or complications related to parathyroid function.
Conclusion:
This case demonstrates the importance of a comprehensive approach to surgery and diagnosis. Even when a primary diagnosis is clear, incidental findings can significantly alter the management plan. The discovery of a parathyroid adenoma in this patient during thyroidectomy serves as a reminder of the complexity of head and neck pathologies. A multidisciplinary approach, careful preoperative evaluation, and histopathological review are essential to ensuring the best outcomes for patients.
Gallery