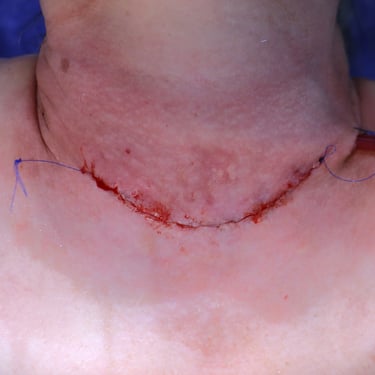
Management of a 58-Year-Old Female with Recurrent Multinodular Goiter (MNG)
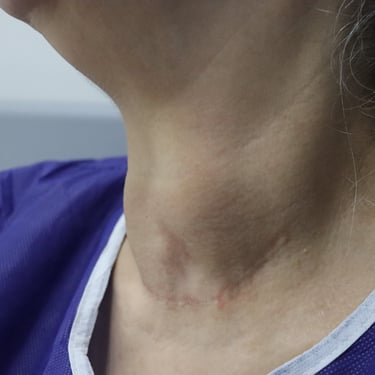
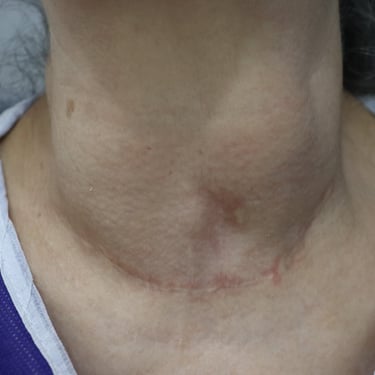
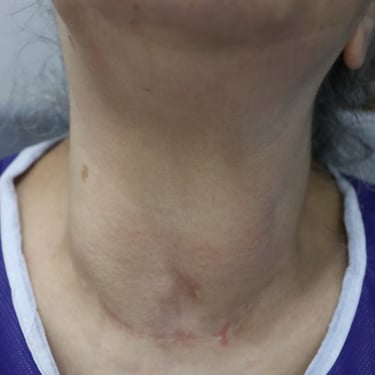
A 58-year-old female presented for post-thyroid surgery follow-up. She has diabetes mellitus, and she is on treatment. She had a thyroid operation in 2003.
SURGERYHEAD AND NECK
9/4/20242 min read
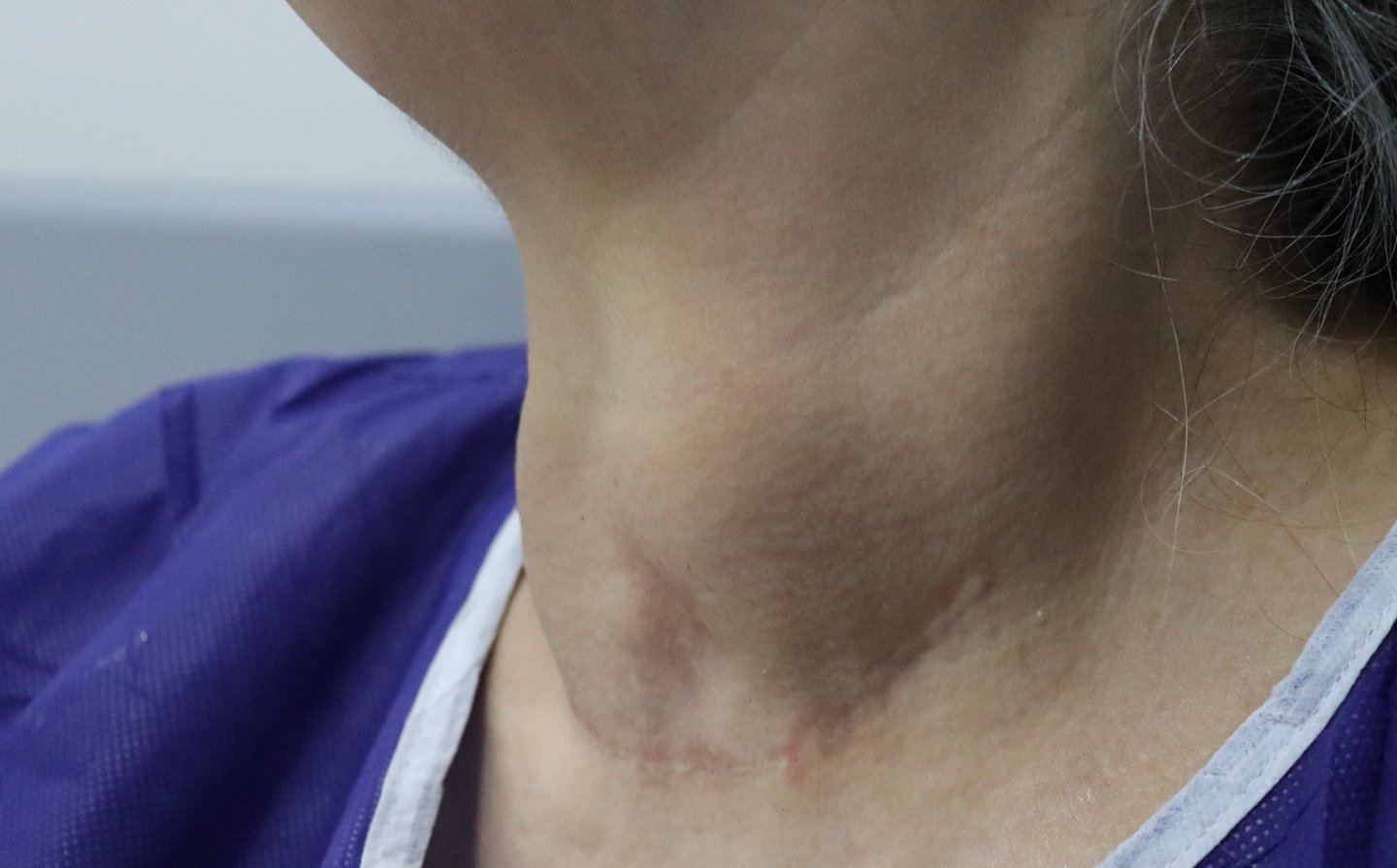
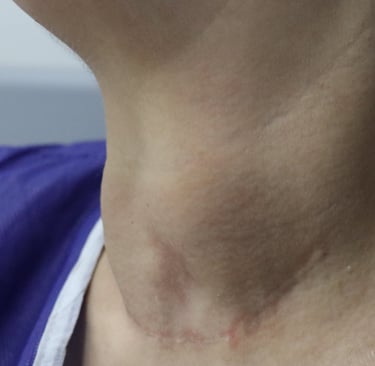
Case Study: Management of a 58-Year-Old Female with Recurrent Multinodular Goiter (MNG)
Patient Presentation:
A 58-year-old female presented for post-thyroid surgery follow-up. She had a history of thyroid surgery in 2003 and is known to have diabetes mellitus, which is managed with medication.
Laboratory Details:
Investigations revealed the following parameters:
Thyroid-stimulating hormone (TSH): 0.646 µIU/mL (normal range: 0.4 - 4.2 µIU/mL)
Free T4: 16.8 pmol/L (normal range: 12 – 22 pmol/L)
Serum Calcium: 9.47 mg/dL (normal range: 8.8 - 10.2 mg/dL)
Hemoglobin A1C (HbA1c): 10.1%
Imaging Findings:
Neck Ultrasound:
The right lobe measured 54 × 33 × 34 mm, and the left lobe measured 55 × 31 × 30 mm, with a 7 mm isthmus thickness.
The thyroid gland was mildly enlarged with heterogeneous echotexture containing multiple well-defined nodules of variable sizes.
Largest nodule (right lobe): 32 × 25 × 20 mm (TI-RADS 3).
Largest nodule (left lobe): 30 × 27 × 25 mm (TI-RADS 3).
Macrocalcifications were observed, with mild increased vascularity and no high-suspicion nodules or retrosternal extension.
Computed Tomography (CT) Scan:
Recurrent, enlarged, nodular thyroid tissue was evident.
Right lobe: 6 × 3.5 × 3.5 cm; Left lobe: 6 × 4.5 × 2.5 cm.
No retrosternal extension was seen.
A 1 cm midline nodule and a 0.7 cm nodule anterior to the thyroid cartilage were identified above the thyroid gland.
Treatment Strategy:
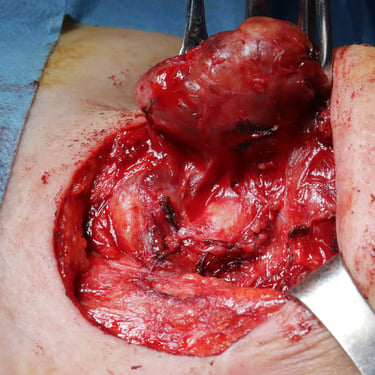
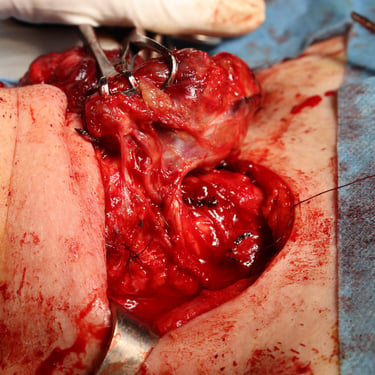
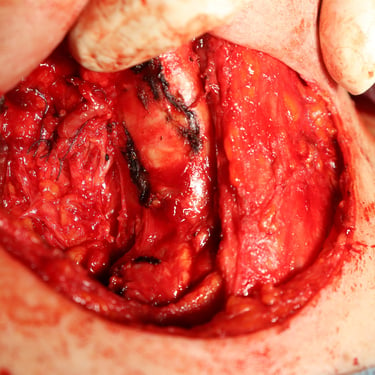
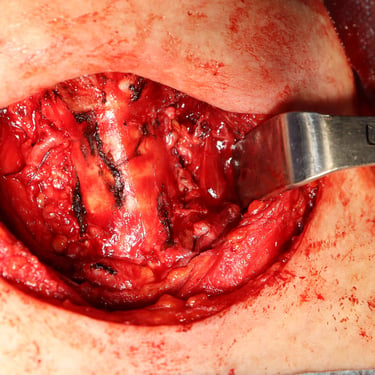
Given the findings of recurrent multinodular goiter, the patient underwent a completion total thyroidectomy.
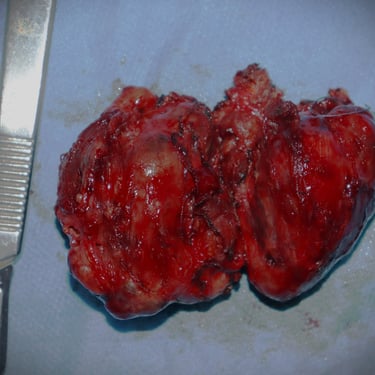
Histopathological Examination (HPE):
Histopathological analysis revealed thyroid tissue with multiple nodules of various sizes. These nodules were composed of benign follicles lined by follicular epithelial cells and filled with colloid material, arranged as macrofollicles. Additional findings included cystic changes, benign papillary hyperplasia, hemorrhage, fibrosis, and calcifications, consistent with thyroid follicular nodular disease with benign secondary changes.
Discussion:
This case highlights the challenges of managing recurrent multinodular goiter, particularly in patients with a history of prior thyroid surgery. The combination of clinical, biochemical, and imaging findings facilitated the decision for surgical intervention. Histopathological evaluation confirmed the benign nature of the nodular disease.
Conclusion:
Completion total thyroidectomy was successfully performed, addressing the recurrence. Regular follow-up is essential to monitor thyroid function, manage diabetes, and evaluate for potential complications or further recurrence.
Gallery: