Neurofibroma of the Tongue in a 14-Year-Old Female
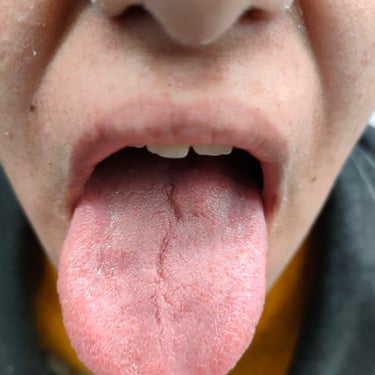
A 14-year-old female presented with a raised, non-ulcerating lesion on the posterior tongue. She had no significant past medical or surgical history. On clinical examination, the lesion was soft and non-fluctuant, with no associated cervical lymphadenopathy. Neurological evaluation was normal, with no focal deficits or abnormalities in other systems.
HEAD AND NECK
12/9/20231 min read
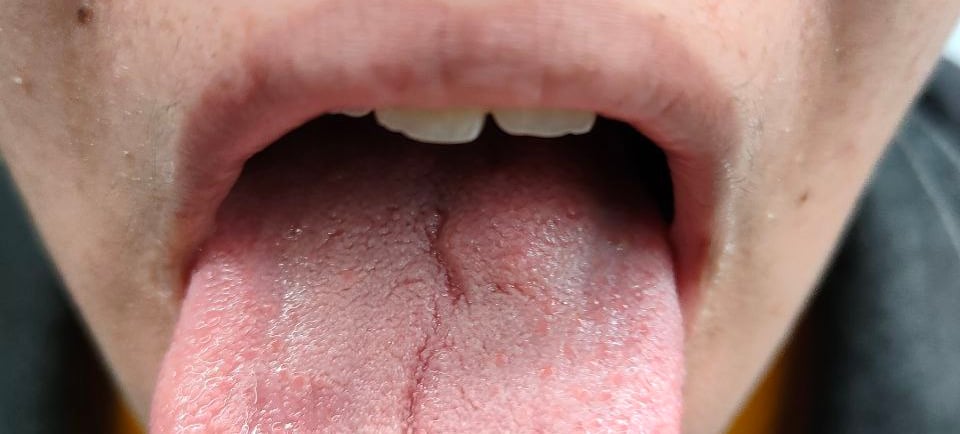
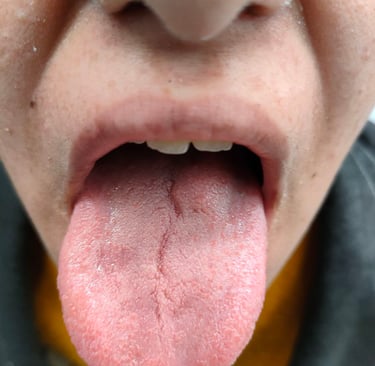
Case Presentation:
A 14-year-old female presented with a raised, non-ulcerating lesion on the posterior tongue. She had no significant past medical or surgical history. On clinical examination, the lesion was soft and non-fluctuant, with no associated cervical lymphadenopathy. Neurological evaluation was normal, with no focal deficits or abnormalities in other systems.
Imaging Findings:
Brain MRI revealed a small area of minimally increased signal intensity on T1-weighted imaging and high signal intensity on T2 and FLAIR sequences, localized to the posterior limb of the left internal capsule and left globus pallidus. There was no surrounding edema, restricted diffusion, or post-contrast enhancement. These findings were possibly consistent with unidentified bright objects (UBOs) seen in neurofibromatosis type I (NF1). The cerebral grey and white matter appeared normal.
Management Plan:
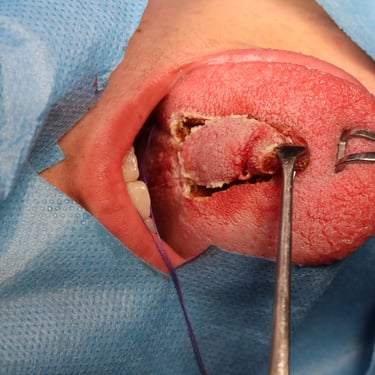
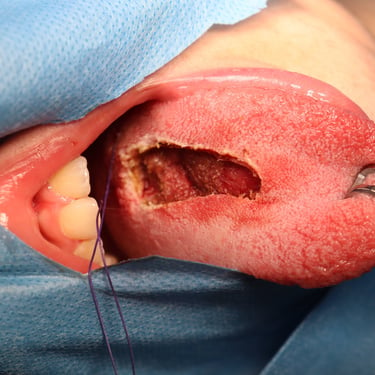
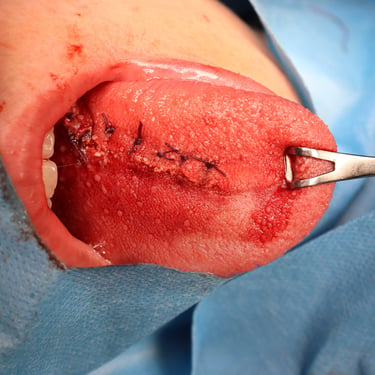
The patient underwent a wide local excision (WLE) of the tongue lesion with primary closure. The surgical procedure was uneventful, and no complications such as tongue deviation or neurological deficits were observed postoperatively.
Histopathological Findings:
Microscopic examination of the excised lesion confirmed the diagnosis of neurofibroma.
Follow-Up and Prognosis:
The patient was scheduled for regular postoperative follow-ups to monitor wound healing and assess for potential recurrence. Long-term surveillance was planned to evaluate for any new neurological symptoms or additional manifestations suggestive of NF1 progression. Given the association between neurofibromas and NF1, genetic counselling and further clinical assessment may be considered if additional features develop.
Gallery