Papillary Thyroid Carcinoma (PTC) Arising from Thyroglossal Duct Cyst (TGDC)
A 33-year-old female presented with a 2-month history of anterior neck swelling. The swelling was painless and not associated with symptoms such as difficulty swallowing, hoarseness, or systemic complaints. She reported no significant past medical or surgical history.
SURGERYHEAD AND NECK
1/30/20252 min read
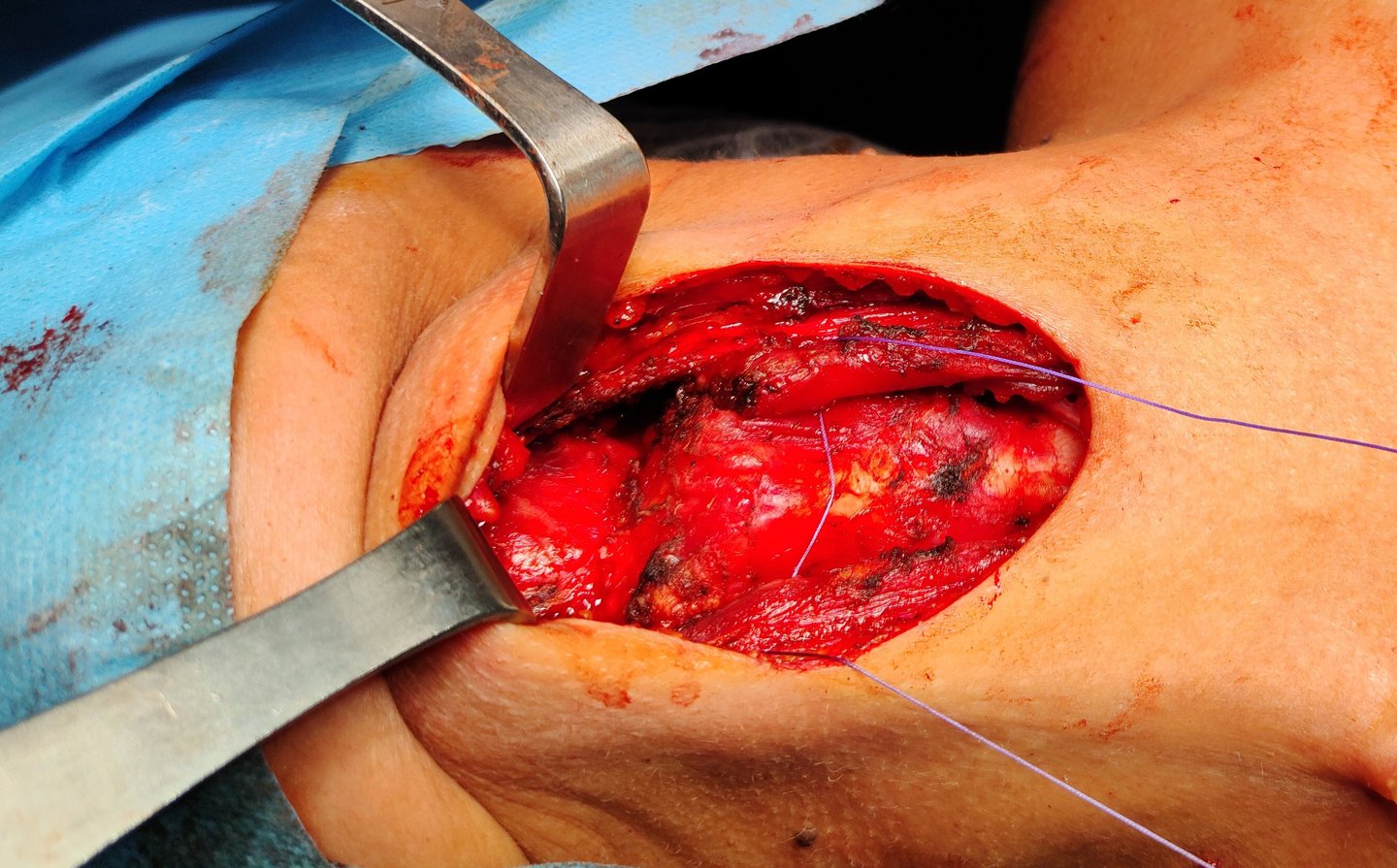
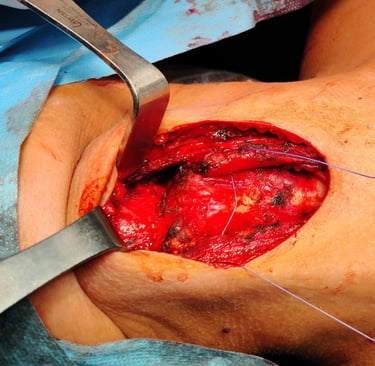
Case Presentation:
A 33-year-old female presented with a 2-month history of anterior neck swelling. The swelling was painless and not associated with symptoms such as difficulty swallowing, hoarseness, or systemic complaints. She reported no significant past medical or surgical history.
Clinical Findings:
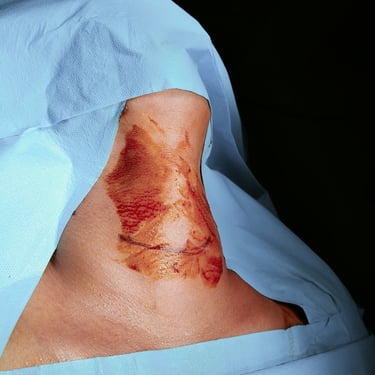
On examination, there was a palpable anterior neck swelling without tenderness, erythema, or overlying skin changes. There was no palpable cervical lymphadenopathy, and her general examination was unremarkable.
Laboratory Investigations:
Thyroid function tests (TFT) revealed a normal thyroid-stimulating hormone (TSH) level of 3.67 μIU/mL and a free thyroxine (FT4) level of 13.59 pmol/L, indicating euthyroid status. Anti-thyroid peroxidase antibody (ATPO) was negative, measuring 8.69 IU/mL.
Imaging Findings:
Neck ultrasound showed a single well-defined, mixed nodule measuring 13 x 8 x 7 mm in the right thyroid lobe, classified as TI-RADS 2. Additionally, a well-defined, mixed hypoechoic nodule measuring 6 x 4.8 x 7.8 mm was identified in the midline at the upper border of the thyroid cartilage, likely representing a thyroglossal duct cyst (TGDC) or lymph node (LN). No suspicious cervical lymphadenopathy was noted.
Fine Needle Aspiration (FNA):
FNA of the midline nodule was positive for malignancy, confirming the diagnosis of papillary thyroid carcinoma (PTC), likely arising from the TGDC. FNA of the right thyroid lobe nodule was benign.
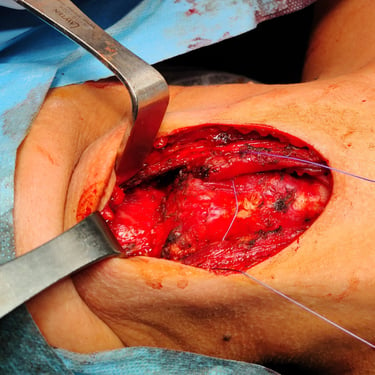
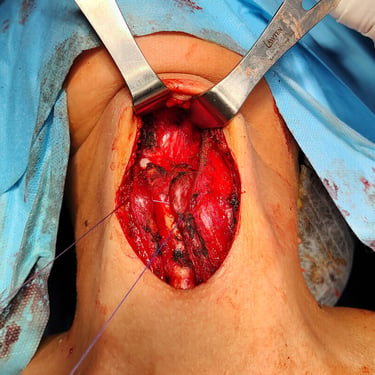
Surgical Intervention:
The patient underwent a total thyroidectomy to address any potential thyroid involvement and enable postoperative radioactive iodine treatment. Additionally, a Sistrunk procedure was performed to completely excise the TGDC along with its tract and the central portion of the hyoid bone.
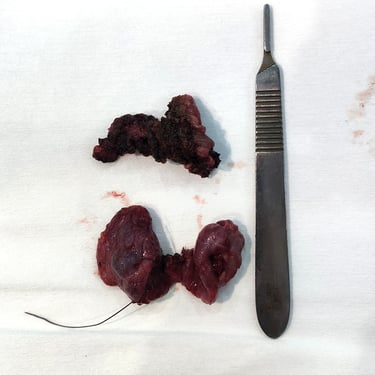
Histopathological Examination (HPE):
Histopathology confirmed the presence of papillary thyroid carcinoma arising within the TGDC. The tumor was well-differentiated, with no evidence of lymphovascular or perineural invasion. Margins were clear of the tumor. The thyroid gland was unremarkable, with no evidence of malignancy.
Postoperative Course:
The patient had an uneventful recovery with no complications such as hypocalcemia, voice changes, or surgical site infection. She was referred for radioactive iodine ablation therapy to address any potential residual disease. Postoperative thyroglobulin levels and TSH were monitored as part of her follow-up care.
Discussion:
Papillary thyroid carcinoma (PTC) arising from the thyroglossal duct cyst (TGDC) is a rare entity, accounting for less than 1% of all thyroid cancers. TGDC is the most common congenital neck anomaly, but malignant transformation is uncommon. Diagnosis relies on a combination of imaging, cytology, and clinical suspicion. The Sistrunk procedure remains the standard treatment for TGDC, while total thyroidectomy is recommended in cases of confirmed PTC to exclude synchronous thyroid carcinoma and facilitate postoperative management, including radioactive iodine therapy. The prognosis for PTC arising in TGDC is excellent with early detection and appropriate treatment.