Papillary Thyroid Carcinoma with Coexisting Right Branchial Cleft Cyst in a 29-Year-Old Male
A 29-year-old male presented with a right submandibular swelling that had been progressively enlarging over the past five years. The swelling was painless and had no associated symptoms such as dysphagia, dyspnea, hoarseness, or systemic signs of infection. The patient’s past medical and surgical history was unremarkable, and there was no known family history of thyroid disease or neck masses.
SURGERYHEAD AND NECKVIDEO
6/14/20253 min read


Patient Presentation:
A 29-year-old male presented with a right submandibular swelling that had been progressively enlarging over the past five years. The swelling was painless and had no associated symptoms such as dysphagia, dyspnea, hoarseness, or systemic signs of infection. The patient’s past medical and surgical history was unremarkable, and there was no known family history of thyroid disease or neck masses.
Laboratory Investigations:
Routine laboratory investigations were performed to assess the patient’s baseline thyroid function and inflammatory status. The erythrocyte sedimentation rate (ESR) was within normal limits at 2 mm/hr. Thyroid-stimulating hormone (TSH) was 2.41 uIU/ml, and free thyroxine (FT4) was 13.0 pmol/L, indicating a euthyroid state. C-reactive protein (CRP) was also low at 0.590 mg/L, suggesting no active systemic inflammation.
Imaging Findings:
Neck ultrasonography revealed a large complex cystic mass in the right upper neck, partially covered by the anterior border of the right sternocleidomastoid (SCM) muscle. The mass measured approximately 74 × 63 × 48 mm, exhibited a thin wall (~1 mm), contained abundant internal echoes, and demonstrated mild lobulation of its inferior surface. It was hypovascular and exerted a posterior-medial displacement of the right common carotid artery (CCA), along with significant compression of the proximal right internal jugular vein (JV). These findings were most consistent with a complicated branchial cleft cyst.
Additionally, the thyroid gland appeared normal in size and echotexture bilaterally. The right lobe measured 52 × 20 × 19 mm, and the left lobe 50 × 19 × 18 mm, with a 4 mm isthmus. However, both lobes harbored single TR4 nodules. The right lobe contained a well-defined, solid, hypoechoic nodule in the lower third measuring 11 × 8 × 7 mm, without calcifications but with increased perinodular and intranodular vascularity. The left lobe contained a similar mid-to-lower third TR4 nodule measuring 16 × 14 × 11 mm.
Fine Needle Aspiration (FNA) and Diagnosis:
An ultrasound-guided FNA was performed on the right thyroid nodule (TR4). Cytological analysis yielded a result of positive for malignancy, consistent with papillary thyroid carcinoma (Bethesda category VI).
Surgical Intervention:
In light of the FNA-confirmed malignancy and the presence of a large right cervical cyst, the patient was scheduled for a combined surgical procedure consisting of total thyroidectomy and excision of the right branchial cleft cyst. Under general anesthesia, a collar incision was performed with elevation of upper and lower skin flaps and division of the strap muscles. The right cervical cyst was identified and excised first, followed by a total thyroidectomy. Palpable cervical lymph nodes were removed and sent for histopathological examination. The left recurrent laryngeal nerve (RLN) and parathyroid glands were preserved. Hemostasis was achieved, a surgical drain was placed, and the wound was closed in layers.
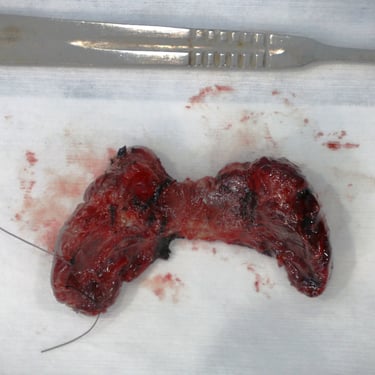
Histopathological Examination (HPE):
Histopathological analysis confirmed a diagnosis of papillary carcinoma of the thyroid gland, conventional type, along with a right branchial cleft cyst. The thyroid malignancy was multifocal, with three tumors identified: one tumor (1.0 cm) in the right lobe and two tumors (1.5 cm and 0.2 cm) in the left lobe. The tumors were well-differentiated, with no lymphovascular or perineural invasion, no extra-thyroidal extension, and no tumor necrosis. A sparse lymphocytic reaction was observed. The parathyroid gland attached to the right lobe was free of tumor. Eight cervical lymph nodes, including three near the cyst, were isolated, all of which were free of malignancy. The excised right cervical cyst was confirmed to be a branchial cleft cyst. The pathological stage according to the AJCC 8th edition was pT1b(m) N0.
Postoperative Management and Follow-Up:
The patient tolerated the surgical procedure well and was monitored postoperatively for potential complications such as hypocalcemia and recurrent laryngeal nerve dysfunction. Given the multifocal papillary thyroid carcinoma without lymph node involvement or extra-thyroidal extension, the patient was classified as low to intermediate risk for recurrence. Long-term follow-up will include periodic surveillance with serum thyroglobulin levels and neck ultrasonography. The prognosis is generally favorable, given the absence of invasive features and nodal metastasis.