Papillary Thyroid Carcinoma with Thyroglossal Duct Cyst Malignancy in a 49-Year-Old Male
A 49-year-old male presented with a one-year history of anterior neck swelling. He was a non-smoker with no significant past medical history except for a previous hernia surgery. He had no history of medication use and no family history of thyroid disease or malignancy.
SURGERYHEAD AND NECK
6/14/20252 min read
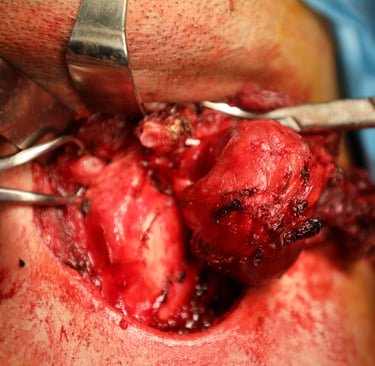
Patient Information:
A 49-year-old male presented with a one-year history of anterior neck swelling. He was a non-smoker with no significant past medical history except for a previous hernia surgery. He had no history of medication use and no family history of thyroid disease or malignancy.
Laboratory Investigations:
Thyroid function tests showed a TSH level of 0.553 µIU/mL, FT4 of 21.5 pmol/L, and total T3 of 1.34 ng/mL, indicating normal thyroid function. The TSH receptor antibody (TRAb) level was 0.964 IU/L, within the normal range.
Neck Ultrasound Findings:
Ultrasound revealed a normal-sized right thyroid lobe (54 × 18 × 16 mm) with multiple small nodules, the largest being a 4.8 × 4 × 4 mm hypoechoic nodule with macrocalcifications (TI-RADS 5). The left thyroid lobe was enlarged (78 × 45 × 30 mm) due to a large TR4 solid isoechoic nodule with microcalcifications, along with a smaller 20 mm TR3 nodule in the lower third.
Additionally, a complex cystic mass (50 × 42 × 21 mm) with a solid mural nodule (12 mm) showing hypervascularity and microcalcifications was seen in the midline neck, extending from the inferior end of the hyoid bone to the left side, raising suspicion for malignancy arising from a thyroglossal duct cyst (TGDC) or the pyramidal lobe. Small, bilateral, lateral cervical lymph nodes were noted, all preserving normal architecture without suspicious features, the largest being 15 × 4 mm in the left level III region.
Neck and Chest CT Findings:
A cystic mass with an enhancing solid component was confirmed in the anterior neck, consistent with a complicated thyroglossal duct cyst requiring tissue diagnosis. No cervical lymphadenopathy, intracranial, or intrapulmonary pathology was detected.
Fine Needle Aspiration (FNA) Cytology:
FNA was performed on the bilateral thyroid nodules and central cystic lesion, yielding the following results:
Right thyroid lobe nodule and central cystic lesion: Positive for malignancy (Bethesda VI), consistent with papillary thyroid carcinoma (PTC).
Left thyroid lobe nodule: Non-diagnostic (Bethesda I) due to hypocellular smear.
Preoperative Investigations and Surgical Management:
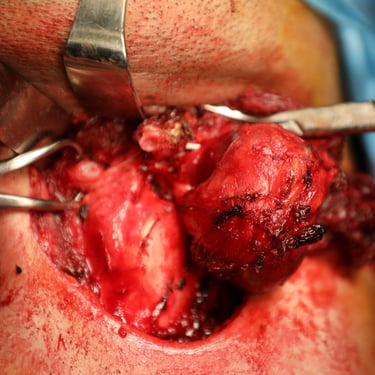
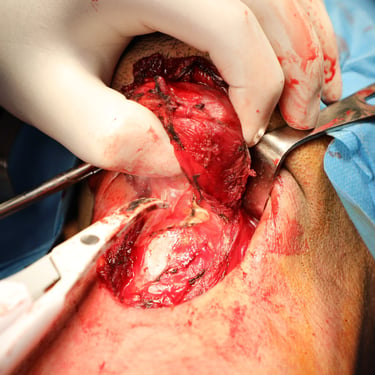
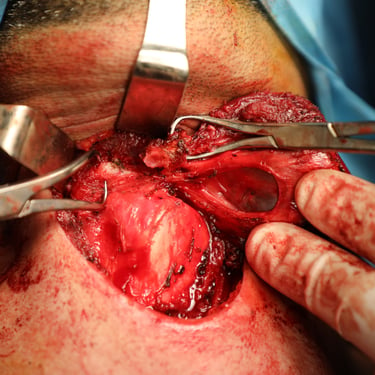
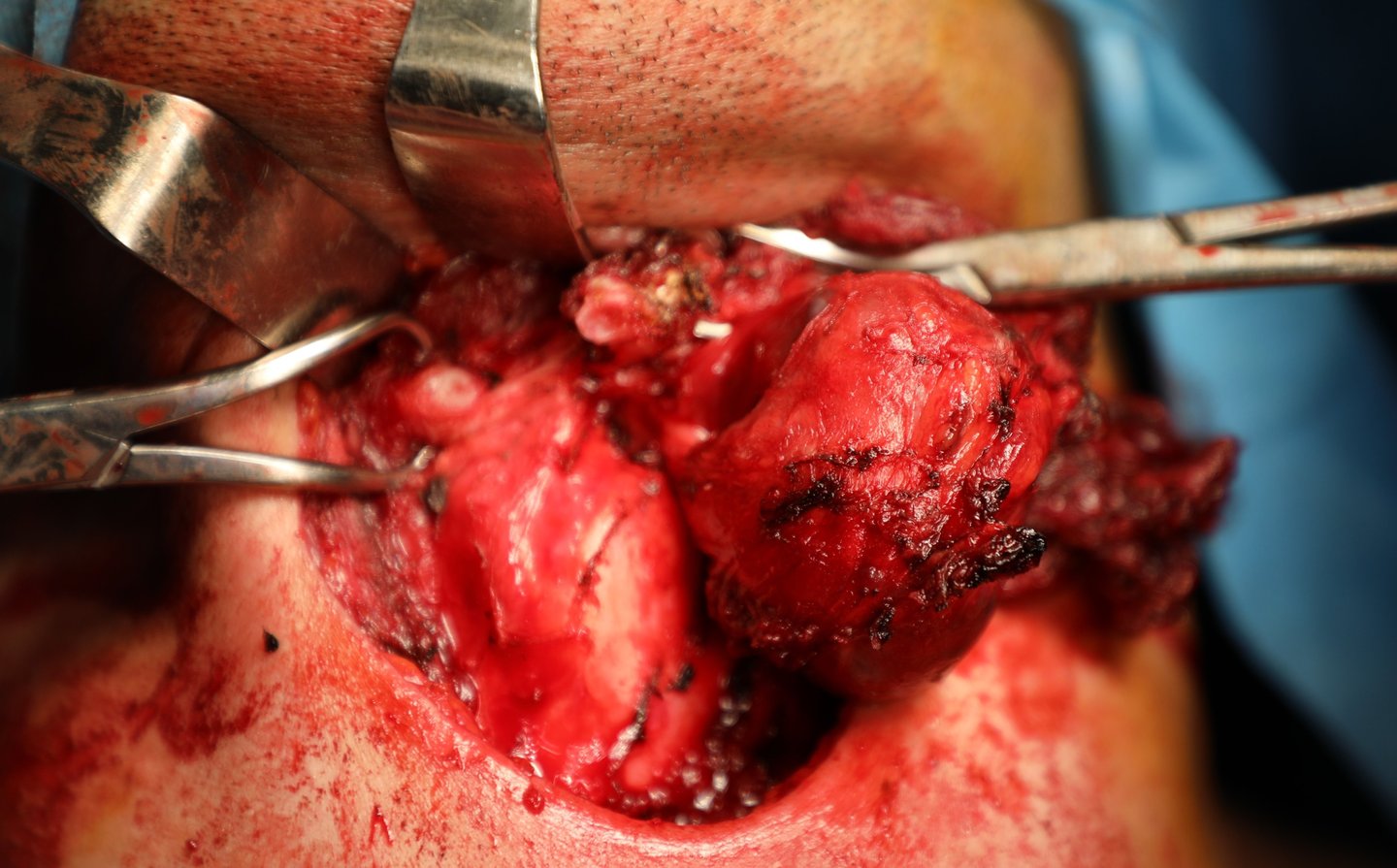
Preoperative thyroglobulin (Tg) was >500 ng/mL, and calcitonin was 4.67 pg/mL, ruling out medullary thyroid carcinoma. The patient underwent total thyroidectomy with Sistrunk procedure, including resection of the thyroglossal duct cyst and overlying strap muscles.
Histopathology Report and Final Diagnosis:
Histopathological analysis confirmed multifocal papillary thyroid carcinoma (PTC) of the conventional subtype, arising in both thyroid lobes and the thyroglossal duct cyst.
Right lobe tumors: 0.6 cm and 0.4 cm.
Left lobe tumor: 4.4 cm.
Thyroglossal duct cyst tumor: 1.4 cm, confined within the cyst without extrathyroidal extension.
Lymphovascular invasion and perineural invasion were not identified.
A single small parathyroid gland (0.1 cm) near the right lobe was tumor-free.
Postoperative Investigations and Follow-Up:
Postoperative lab results showed:
TSH: 1.42 µIU/mL
FT4: 17.7 pmol/L
Tg: 7.94 ng/mL (for postoperative monitoring)
PTH: 32.5 pg/mL (within normal range)
Calcium: 9.03 mg/dL (normal)
The patient had an uneventful postoperative recovery and was advised long-term follow-up with thyroglobulin monitoring to assess for recurrence.
Gallery