Parathyroid Carcinoma and Papillary Thyroid Carcinoma in a Case of Recurrent Multinodular Goiter
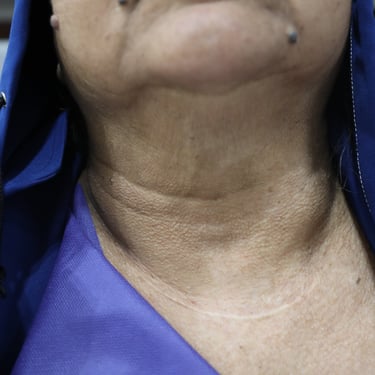
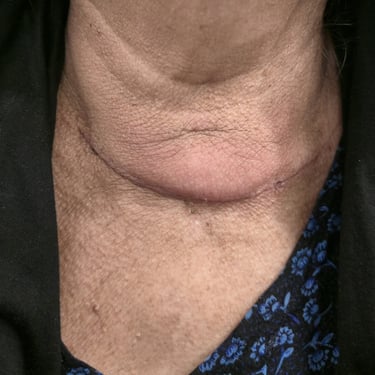
A 70-year-old female presented for abdominal pain for one month duration, associated with a history of thyroid nodules and biochemical hyperparathyroidism. She was a known case of recurrent multinodular goiter, having undergone thyroid surgery approximately 30 years ago for a benign condition. On neck examination, there was noticeable thyroid enlargement. She had no history of renal stones, although renal function tests showed elevated levels, and both serum calcium and PTH were markedly increased.
SURGERYHEAD AND NECKVIDEO
6/25/20252 min read


Clinical Presentation:
A 70-year-old female presented for abdominal pain for one month duration, associated with a history of thyroid nodules and biochemical hyperparathyroidism. She was a known case of recurrent multinodular goiter, having undergone thyroid surgery approximately 30 years ago for a benign condition. On neck examination, there was noticeable thyroid enlargement. She had no history of renal stones, although renal function tests showed elevated levels, and both serum calcium and PTH were markedly increased.
Laboratory Investigations:
Thyroid function tests were within normal limits with a TSH of 1.47 uIU/ml and FT4 of 16.5 pmol/L. However, there was severe hypercalcemia (serum calcium 16.6 mg/dL) and markedly elevated PTH (1050 pg/ml), consistent with primary hyperparathyroidism. Renal function was mildly impaired with creatinine at 1.27 mg/dL and urea at 29.4 mg/dL. HbA1c was elevated at 7.59%, and serum calcitonin was mildly elevated at 1.79 pg/ml.
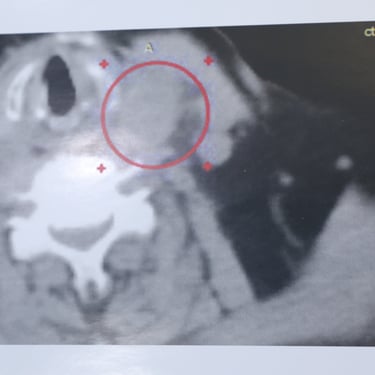
Neck Imaging:
Ultrasound showed significant enlargement of both thyroid remnants. The right lobe measured 56 × 43 × 30 mm and the left 60 × 38 × 35 mm. The thyroid tissue was heterogenous with multiple well-defined nodules of various sizes. The largest nodules were TR3 in category, measuring 48 × 42 × 25 mm (right) and 36 × 30 × 27 mm (left). Mildly increased vascularity and macrocalcifications were noted. Mild left-sided retrosternal extension was observed. Additionally, an intrathyroidal solid hypoechoic nodule with partial retrosternal extension on the left side raised suspicion of either a TR4 thyroid nodule or parathyroid adenoma. Subsequent parathyroid scintigraphy supported the diagnosis of a parathyroid lesion.
Surgical Management:
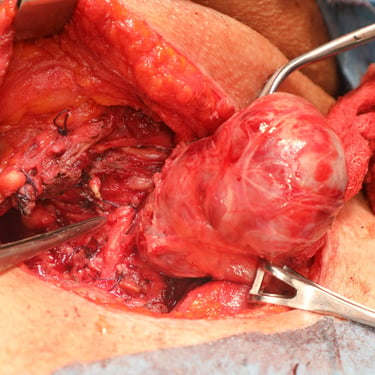
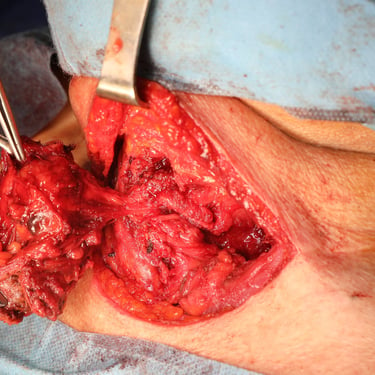
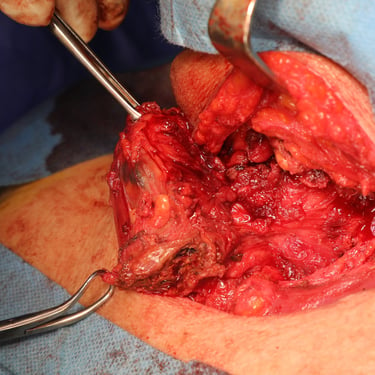
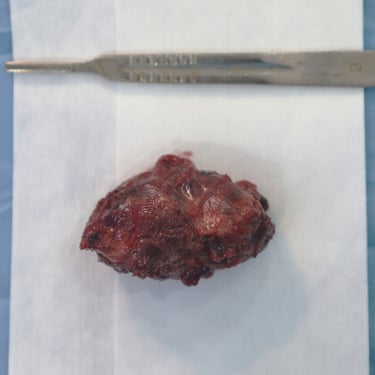
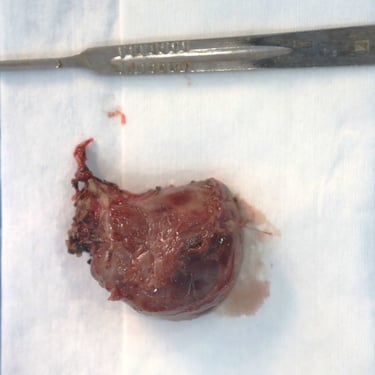
The patient was prepared for surgery and underwent a total thyroidectomy with excision of suspected parathyroid tissue. The procedure was done under general anesthesia in a supine, neck-extended position. Through a collar incision, total thyroidectomy was performed, along with removal of the left intrathyroidal parathyroid lesion and a suspicious right lower neck mass. Left RLN and PTGs were identified; however, safety of the left RLN was uncertain intraoperatively. Hemostasis was secured, and a redivac drain was placed. The total operative time was 3 hours. Specimens were labeled and sent in three containers: (1) left lobe with intrathyroidal parathyroid, (2) right lobe, and (3) right lower neck mass.
Postoperative Course:
Postoperative serum calcium was initially elevated at 14.8 mg/dL, but showed a downward trend over the next two days (12.7 mg/dL, then 11.9 mg/dL). One month after surgery, ENT evaluation revealed left vocal cord palsy and limited movement of the right vocal cord. Thyroid function at that time remained within normal range (TSH 2.46 uIU/ml, FT4 19.0 pmol/L).
Histopathology:
Final histological analysis revealed multiple pathologies:
Thyroid Gland: The thyroidectomy specimen showed a unifocal 1.8 cm conventional papillary thyroid microcarcinoma in the right lobe with lymphovascular and perineural invasion. No extrathyroidal extension was noted. Three right lower neck lymph nodes were positive for metastatic papillary carcinoma with extranodal extension. Final staging was pT1b N1b. The background thyroid tissue showed follicular nodular disease with focal lymphocytic thyroiditis.
Right Neck Mass: Confirmed as metastatic papillary thyroid carcinoma involving all three dissected lymph nodes with extranodal extension. Largest metastatic focus was 0.8 cm.
Left Intrathyroidal Nodule: Diagnosed as parathyroid carcinoma, showing capsular infiltration and extensive vascular invasion (more than four foci). Tumor was at least 3 cm in size (disrupted). Focal necrosis and atypia were noted, with a sparse lymphocytic reaction. No perineural invasion was observed. Final staging was pT2 N0.