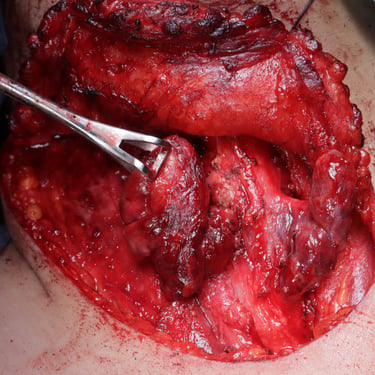
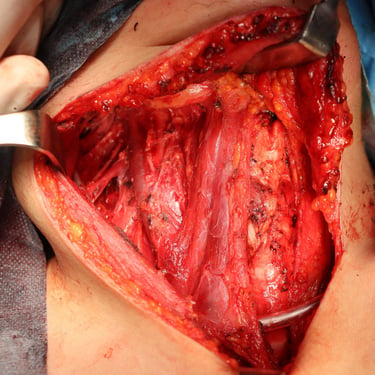
PTC: Total Thyroidectomy and Central and Lateral LN Neck Dissection
Management of a 27-Year-Old Female with Papillary Thyroid Carcinoma and Cervical Lymph Node Metastasis
SURGERY
7/9/20242 min read
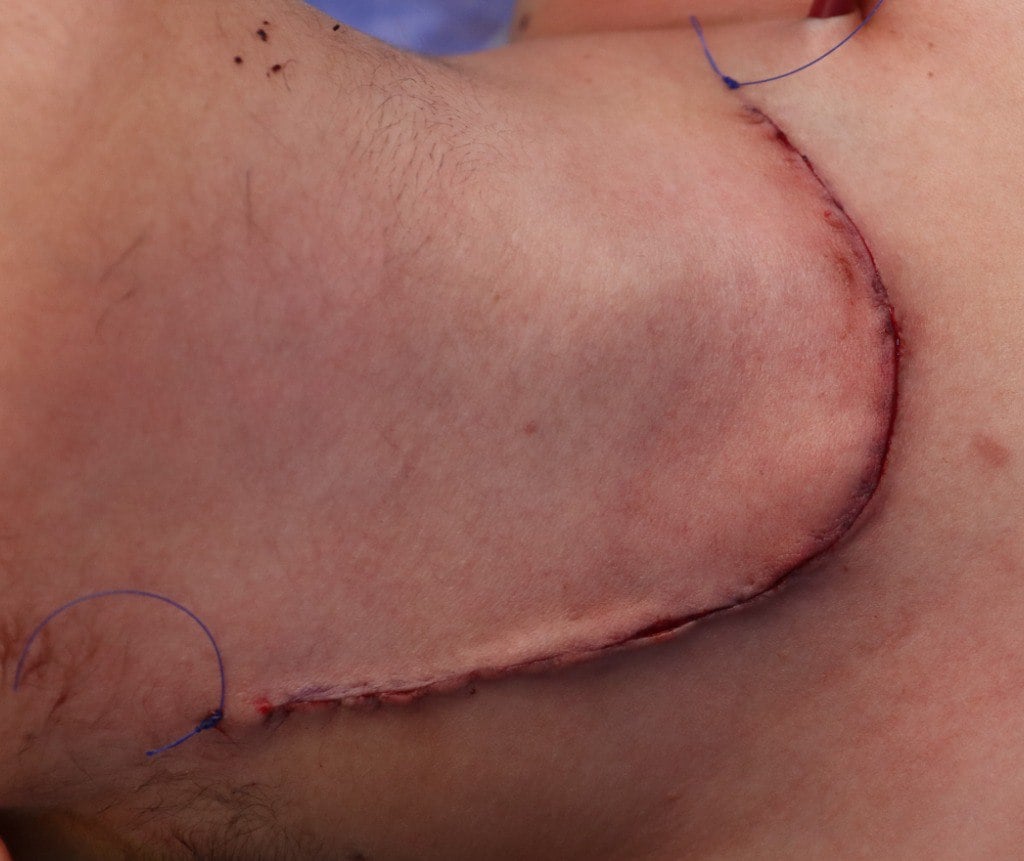
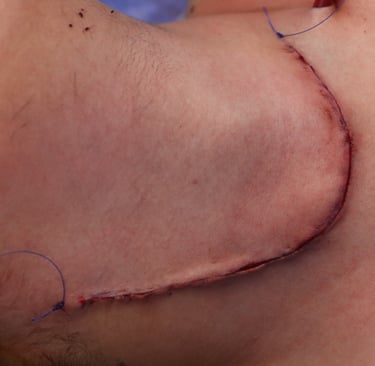
Case Presentation:
A 27-year-old female presented with a one-week history of neck pain and swelling on the right side. She described the swelling as firm, with a sensation of discomfort and pressure in the neck area. There were no associated symptoms such as difficulty in breathing or swallowing. The patient had no significant past medical or surgical history, no history of thyroid disease, and was not on any regular medications. There was no significant family history of thyroid disease or cancer, and she was a non-smoker.
General Examination:
Patient was alert and oriented, with stable vital signs.
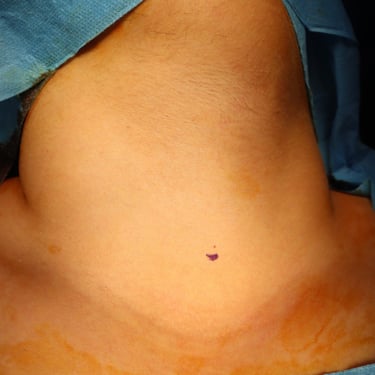
Neck Examination:
Palpable swelling on the right side of the neck. The right thyroid lobe was enlarged and firm.
Investigations:
Laboratory Tests:
TSH: 1.75 µIU/mL
FT4: 23.5 pmol/L
Thyroglobulin: 0.137 ng/mL
Serum Calcium: 7.38 mg/dL
Neck Ultrasound Findings:
Right Thyroid Lobe: A well-defined, solid isoechoic nodule measuring 11 x 8 x 8.7 mm with microcalcifications and increased perinodular and intranodular vascularity.
Additional Nodules: Two smaller similar nodules present in the right mid-third of the thyroid.
Cervical Lymph Nodes: Multiple suspicious lymph nodes surrounding the gland, with the largest being 16 x 14 mm near the right lower pole (partially retrosternal). Multiple large solid isoechoic hypervascular lymph nodes in the right lateral groups II, III, and IV, with the largest measuring 53 x 21 mm, suggestive of secondary lymph nodes of thyroid origin.
Fine Needle Aspiration Cytology (FNAC):
Right Thyroid Lobe Nodule: Positive for malignancy, Bethesda VI (Papillary Thyroid Carcinoma).
Right Cervical Lymph Node: Positive for malignancy, metastatic papillary thyroid carcinoma.
CT Scan:
No distant metastasis detected.
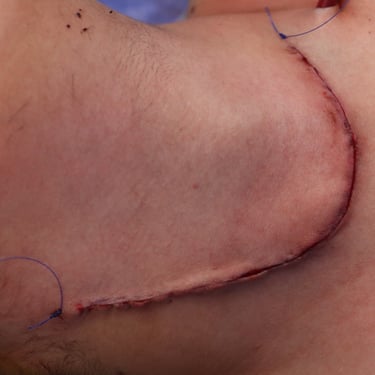
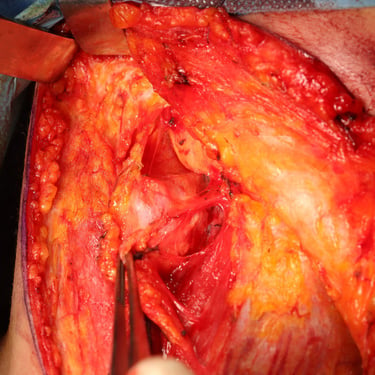
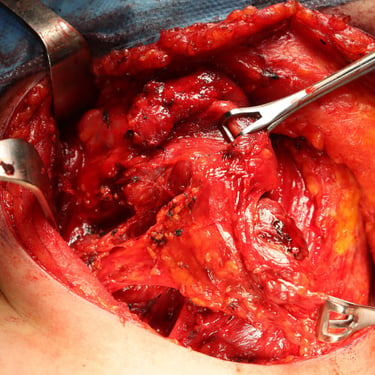
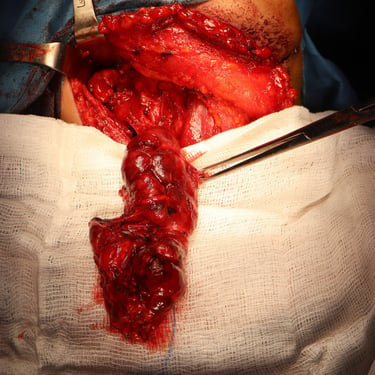
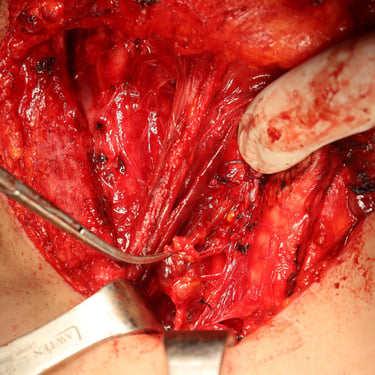
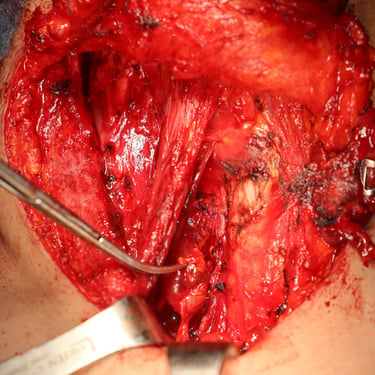
Surgery:
The patient underwent total thyroidectomy with right central and right lateral cervical lymph node dissection.
Post-Surgery Condition:
The patient recovered well without any complications such as hypocalcemia, hoarseness of voice, or chyle leak. Postoperative monitoring showed stable vital signs.
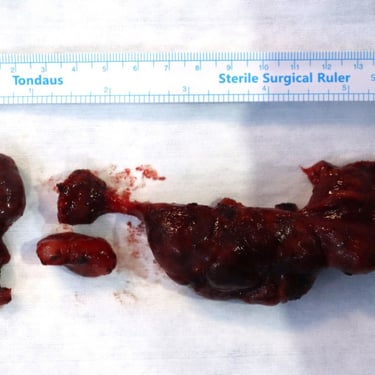
Histopathological Examination (HPE):
Thyroid Gland: Multifocal papillary carcinoma of the right lobe, with three tumors identified. The largest tumor measured 1.2 cm, with two smaller tumors (0.2 cm each) around it.
Tumor Characteristics: Well-differentiated tumors with lymphovascular invasion, perineural invasion, and minimal extrathyroidal extension.
Thyroiditis: Chronic lymphocytic thyroiditis was also noted.
Lymph Nodes: Out of 49 lymph nodes, 13 were involved with extranodal extension, with the largest lymph node deposit measuring 5 cm.
Pathological Stage (AJCC 8th edition):
pT1b(m) N1b
Further Management:
Following surgery, the patient was referred for radioiodine ablation to manage any remaining thyroid tissue or potential microscopic metastasis.
Discussion:
This case highlights the management of papillary thyroid carcinoma (PTC) with cervical lymph node metastasis. PTC is the most common type of thyroid cancer and often presents with cervical lymphadenopathy, as seen in this patient. The decision to perform total thyroidectomy followed by central and lateral neck dissection was appropriate given the presence of metastatic lymph nodes. The histopathological findings, including the identification of multifocal tumors and lymphovascular and perineural invasion, helped in staging the disease as pT1b(m) N1b, guiding the decision for postoperative radioiodine therapy.
The presence of chronic lymphocytic thyroiditis in this case is notable, as it may have impacted the thyroid's immune environment and could be related to the patient's thyroid pathology.
Conclusion:
This case emphasizes the importance of early detection and comprehensive management of thyroid cancer, including both surgical intervention and subsequent radioactive iodine therapy for appropriate staging and treatment. Continuous follow-up is necessary to monitor for recurrence, especially given the lymph node involvement.
Gallery