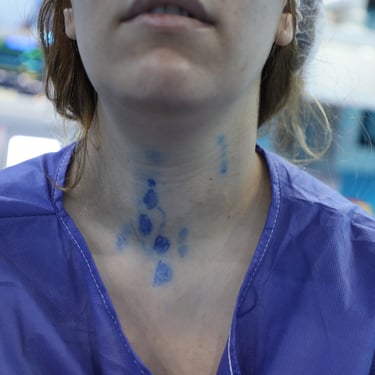Recurrent Papillary Thyroid Carcinoma with Bilateral Lateral Cervical Lymph Node Metastasis
A 35-year-old female presented with a history of thyroid disease of 3 years duration. She had undergone a thyroid operation three years prior for papillary thyroid carcinoma and had received radioactive iodine (RAI) therapy postoperatively. She reported no significant new symptoms at the time of presentation.
SURGERYHEAD AND NECKVIDEO
6/14/20252 min read

Clinical Presentation:
A 35-year-old female presented with a history of thyroid disease of 3 years duration. She had undergone a thyroid operation three years prior for papillary thyroid carcinoma and had received radioactive iodine (RAI) therapy postoperatively. She reported no significant new symptoms at the time of presentation.
Investigations:
Laboratory tests revealed elevated Thyroid-Stimulating Hormone (TSH) at 49.8 uIU/ml and low-normal Free T4 at 10.3 pmol/L, indicating hypothyroidism. Serum calcium was 9.18 mg/dl and parathyroid hormone (PTH) level was 35.5 pg/ml, within normal limits. Calcitonin was <0.500 pg/ml. Thyroglobulin was elevated at 62.6 ng/ml. Renal function tests and complete blood count were within normal limits, and viral screening was negative. Vocal cord examination showed normal mobility, shape, and color of both vocal cords.
Neck Ultrasound Findings:
Ultrasound of the neck showed remnant thyroid tissue in the right lobe operation bed measuring approximately 39 × 18 × 17 mm with inhomogeneous echotexture and multiple solid, hypoechoic, vascular nodules with microcalcifications, consistent with highly suspicious TR5 nodules or metastatic lymph nodes. Similar nodules were noted in the left thyroid bed and in the midline over the trachea extending retrosternally. Additionally, multiple suspicious cervical lymph nodes were identified bilaterally, with microcalcifications and loss of normal hilar architecture. The largest right-sided LN was 16 × 5 mm (group III), and the largest left-sided LN was 12 × 3 mm (group II). Submandibular and parotid glands appeared normal.
Fine Needle Aspiration Results:
FNA of the right TR5 nodule and bilateral cervical lymph nodes confirmed recurrence of papillary thyroid carcinoma. The right thyroid remnant was Bethesda category VI, and both right and left cervical lymph nodes tested positive for metastatic papillary thyroid carcinoma.
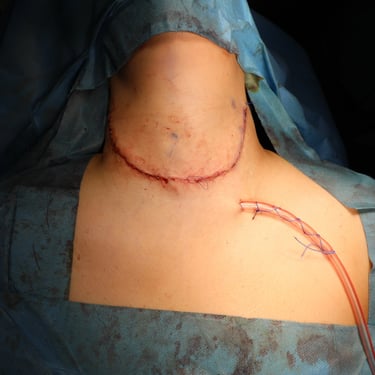
Management and Surgery:
Given the findings, the patient was scheduled for revision thyroid surgery. She underwent recurrent thyroidectomy with bilateral central lymph node dissection (CLND) and bilateral lateral lymph node dissection (LLND). Under general anesthesia, a collar incision was made in the supine, neck-extended position. Total thyroidectomy was performed, preserving both recurrent laryngeal nerves and parathyroid glands. Redivac drains were placed, and the wound was closed in layers. Dissection included bilateral lateral neck groups (levels II–V) and bilateral central compartments. All major vessels and nerves, including the vagus and phrenic nerves, were preserved. The procedure duration was 4 hours and 30 minutes.
Histopathology:
Histological examination confirmed metastatic papillary thyroid carcinoma involving 18 of 65 lymph nodes. Specifically:
Right central group: 11 of 11 nodes involved.
Left central group: 4 of 5 nodes involved.
Right lateral group: 0 of 20 nodes involved.
Left lateral group: 3 of 29 nodes involved.
No residual thyroid tissue was seen; only skeletal muscle and fibrous tissue were identified at the thyroid bed.
Postoperative Course:
The patient tolerated the procedure well with no immediate complications. She was stable postoperatively and scheduled for further oncological evaluation and follow-up.