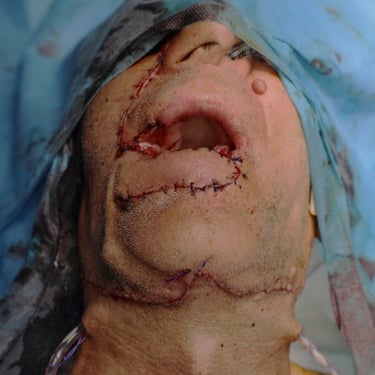
Recurrent Poorly Differentiated Squamous Cell Carcinoma of the Lower Lip in a 66-Year-Old Male
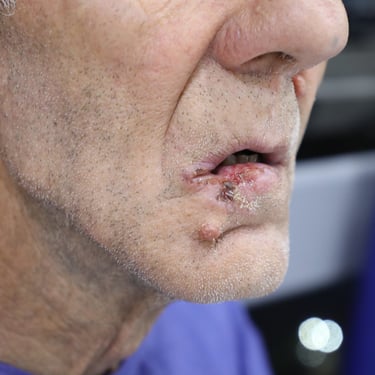
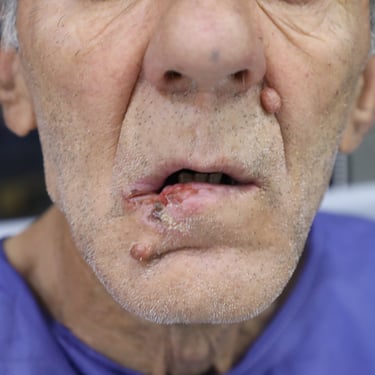
A 66-year-old male presented to the outpatient surgical oncology clinic with a recurrent lesion of the lower lip. He had undergone two previous surgical interventions for a lower lip mass over the past two years, both of which yielded histologically confirmed squamous cell carcinoma (SCC) with involved resection margins. Despite prior interventions, the patient reported persistent recurrence and progressive enlargement of the lesion. He now presented with an advanced, ulcerated lesion involving the right lower lip, causing functional discomfort during speech and eating. The patient has a history of chronic, heavy tobacco use and remains an active smoker. He has no history of diabetes or viral hepatitis. Cardiovascular history includes a recent coronary CT angiogram that showed mild proximal LAD stenosis, but no significant coronary artery disease.
SURGERYHEAD AND NECK
6/17/20253 min read
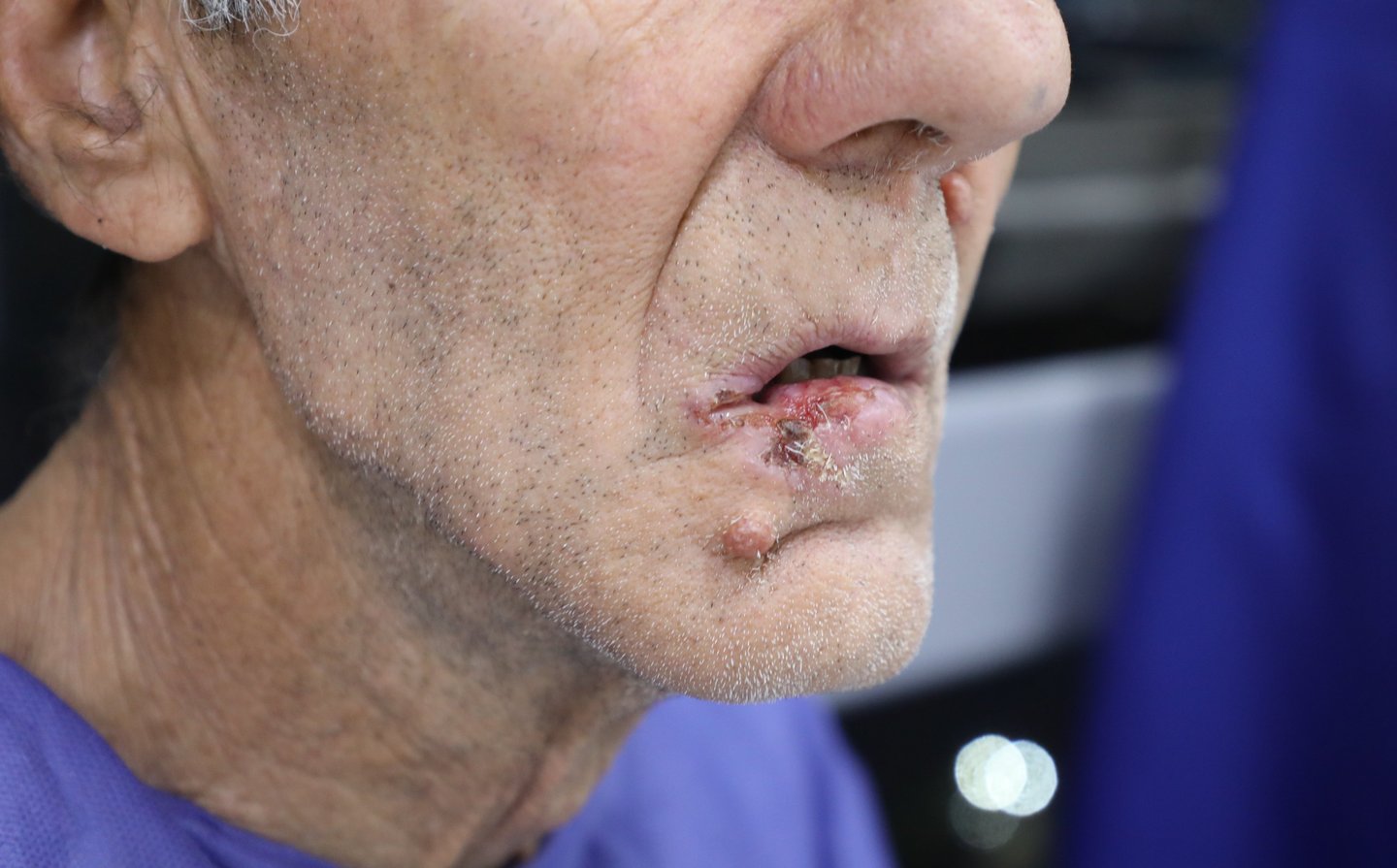
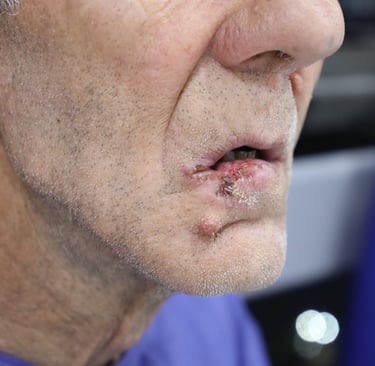
Patient Information:
A 66-year-old male presented to the outpatient surgical oncology clinic with a recurrent lesion of the lower lip. He had undergone two previous surgical interventions for a lower lip mass over the past two years, both of which yielded histologically confirmed squamous cell carcinoma (SCC) with involved resection margins. Despite prior interventions, the patient reported persistent recurrence and progressive enlargement of the lesion. He now presented with an advanced, ulcerated lesion involving the right lower lip, causing functional discomfort during speech and eating. The patient has a history of chronic, heavy tobacco use and remains an active smoker. He has no history of diabetes or viral hepatitis. Cardiovascular history includes a recent coronary CT angiogram that showed mild proximal LAD stenosis, but no significant coronary artery disease.
Laboratory Investigations:
Routine preoperative laboratory tests were unremarkable. Complete blood count (CBC) was within normal limits, and there were no significant inflammatory markers—Erythrocyte Sedimentation Rate (ESR) was measured at 14 mm/hr. Thyroid function tests were normal, with TSH at 1.68 µIU/mL and Free T4 at 15.1 pmol/L. Renal function tests were normal. Viral serology screening was negative for hepatitis B, hepatitis C, and HIV.
Ultrasound Findings:
A neck ultrasound was performed to evaluate the cervical lymphatic spread. Multiple bilateral cervical lymph nodes were noted, particularly in the right lateral groups. These lymph nodes varied in size and location:
Right submandibular: 19 × 5.7 mm
Right group II: 16 × 5 mm
Left group III: 13 × 4 mm
All lymph nodes demonstrated benign ultrasound characteristics, including preserved hilum, smooth margins, and cortical thickness <3 mm. No suspicious features of metastatic involvement were seen.
The ultrasound also detected a solid, irregularly contoured, hypoechoic lesion at the site of the prior surgical scar in the right lower lip, measuring approximately 12 × 10 × 7 mm. The lesion showed mild internal vascularity and was considered suspicious for recurrent SCC. The thyroid gland, parotid glands, and submandibular glands were normal in size and texture, with no evidence of focal lesions.
Preoperative Evaluation and Planning:
Given the clinical suspicion for recurrence and ultrasound findings, the patient was scheduled for surgical resection. His cardiovascular risk was evaluated via coronary CT angiography, which showed only mild stenosis in the proximal LAD and was not a contraindication for surgery.
The surgical plan included: Wide local excision of the right lower lip lesion, Prophylactic right submandibular gland excision and Bilateral lateral cervical lymph node dissection.
Preoperative medications included Potafast (potassium citrate) for urinary alkalinization, likely related to his remote history of nephrolithiasis, and Doreta (tramadol/paracetamol) for pain management. He remained clinically stable preoperatively.
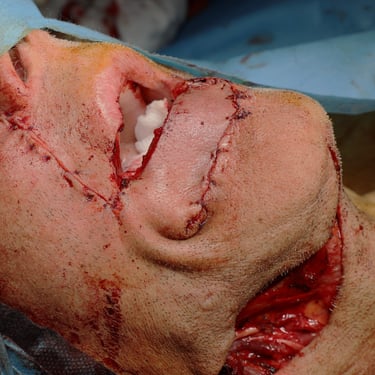
Surgical Intervention:
The patient underwent right lower lip wide local excision, right submandibular gland removal, and bilateral cervical lymphadenectomy under general anesthesia. The procedure was uneventful with adequate hemostasis. The surgical specimen was sent for histopathological analysis.
Histopathological Examination (HPE):
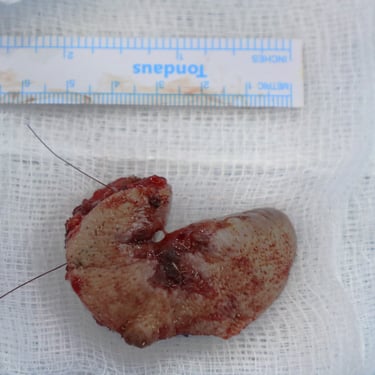
Microscopic examination confirmed the presence of poorly differentiated squamous cell carcinoma (Grade 3). Key features included:
Tumor size: 2.4 cm
Depth of invasion: 1.4 cm, extending into skeletal muscle fibers
Ulceration: Present
Lymphovascular and perineural invasion: Both present
Despite these aggressive histologic features, all resection margins were negative, with the closest being 0.3 cm on the lateral side.
Deep margin: 0.7 cm
Superior (upper lip): 0.4 cm
Medial: 0.6 cm
A total of 77 lymph nodes were examined, and none showed evidence of tumor metastasis. Some nodes contained non-necrotizing granulomas, possibly of reactive or granulomatous etiology.
The right submandibular gland was histologically unremarkable.
Additional findings included solar elastosis and an incidental intradermal nevus.
The final pathologic stage was pT2 pN0, with no nodal involvement and localized but invasive disease.
Postoperative Management and Follow-Up Plan:
Postoperative recovery was smooth. Given the poor differentiation, perineural and lymphovascular invasion, and prior history of margin involvement, the patient is considered at high risk for recurrence despite negative nodal involvement. A multidisciplinary tumor board recommended postoperative adjuvant radiotherapy to the primary site to reduce local recurrence risk.
He was strongly advised to pursue smoking cessation, given its contribution to recurrence and overall morbidity. Long-term surveillance will include regular physical exams, imaging of the neck (US or MRI), and chest imaging due to the risk of distant metastasis in high-grade oral SCCs.
Gallery